COVID-19: Deaths in 2021 were around 1%, or 2,000 more than expected, had there been no pandemic
Catch up on the Actuaries Institute’s COVID-19 Mortality Working Group’s latest analysis of excess deaths.
In summary:
|
![]()
Background
The COVID-19 Mortality Working Group has examined the latest provisional mortality statistics to 31 December 2021, released by the Australian Bureau of Statistics (ABS) on 30 March 2022. We have compared our predicted baseline number of deaths to observed deaths, noting that our detailed analysis by cause of death is based on data for doctor-certified deaths only (excluding roughly 12% of all deaths that are certified by the coroner).
We have also:
- estimated excess mortality for all deaths (not just doctor-certified deaths) for both 2020 and 2021, noting that the information on coroner-referred/total deaths is preliminary and incomplete;
- compared our excess mortality estimates to those produced by the ABS and those included in Our World in Data (OWID); and
- provided an indicative estimate of excess mortality for the first three months of 2022.
 Excess doctor-certified deaths to 31 December 2021
Excess doctor-certified deaths to 31 December 2021
In brief, the Working Group’s analysis:
- scales actual weekly doctor-certified deaths from 2015 to 2020 so that they are representative of the number of deaths in those years if they had the 2021 population size and age mix;
- fits a linear regression model to the scaled deaths from 2015 to 2019, giving overall mortality improvements of around 1.8% per annum over the five-year period;
- extrapolates the linear regression model to arrive at a predicted number of deaths for each week in 2020 and 2021 (assuming that the same 1.8% per annum mortality improvement continues and ignoring the impact of the pandemic); and
- compares predicted deaths to the actual deaths in 2021 (after a small allowance for late reported deaths).
It is important to note that expected deaths are increasing faster from demographic changes (ageing and population size) than they are reducing due to mortality improvement. As a result, our model predicts higher deaths in each successive year. Our prediction for 2021 is higher than for 2020 and both are higher than the 2015-19 average. Thus, despite the overall mortality improvements, our predicted doctor-certified deaths for 2021 are 7,800 (6%) above the 2015-19 average.
The graph and table below summarise the results of the analysis. This article concentrates on the experience in 2021, but we have also shown the 2020 results (scaled to 2021 in the graphs) for context.
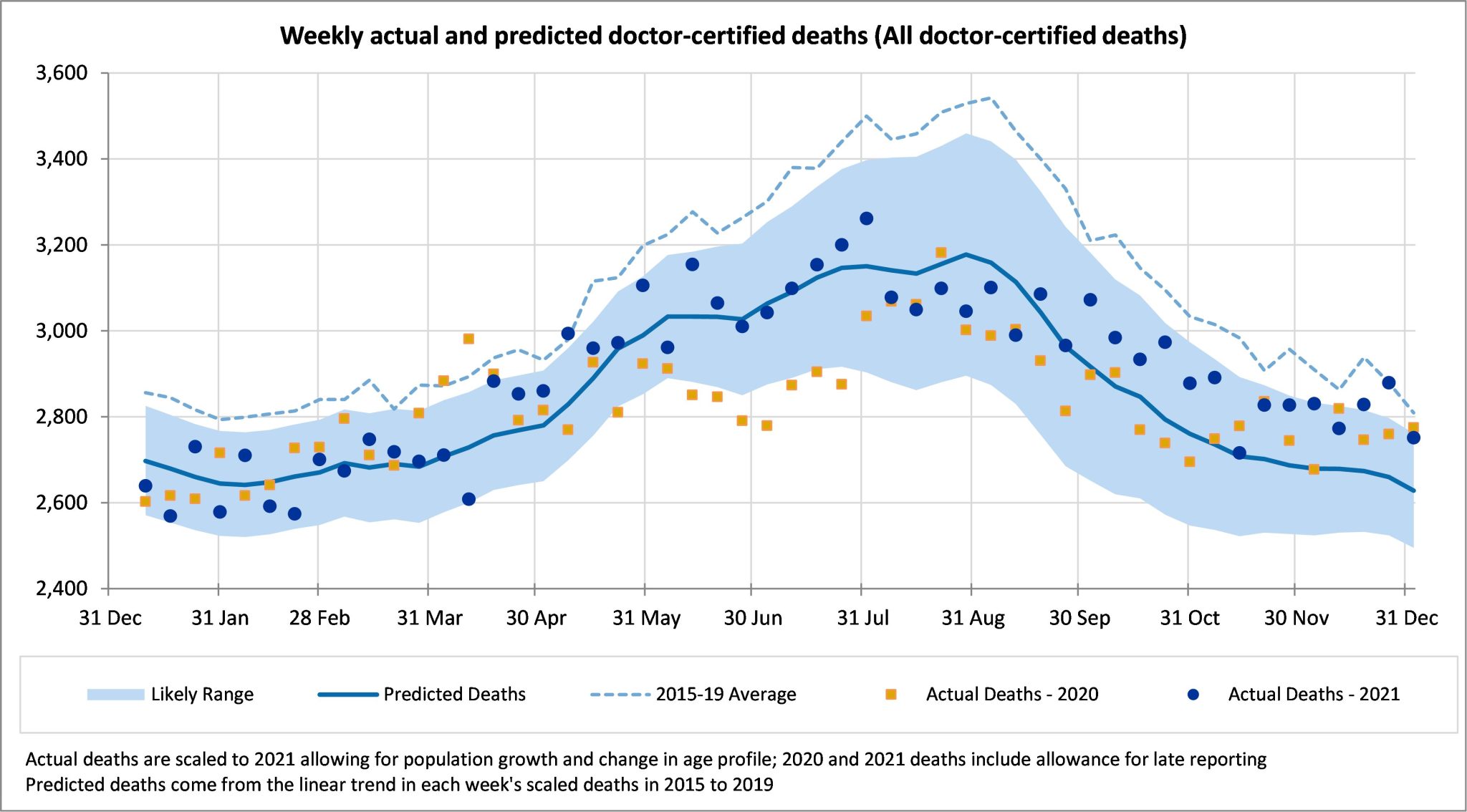
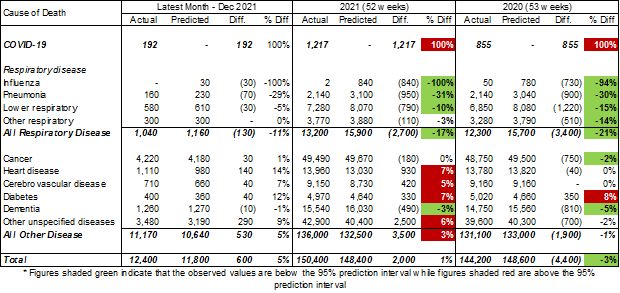
Table 1 – Excess Doctor-certified deaths
|
|
For the month of December 2021, total doctor-certified deaths were 5% (or 600) higher than predicted. Deaths in four of the last five weeks of the year were at or above the upper end of the prediction interval (i.e. above the 97.5th percentile). By cause:
- there were 192 doctor-certified deaths from COVID-19;
- deaths from respiratory disease continued to be lower than expected (down 11% or 130);
- deaths from heart disease, cerebrovascular disease, diabetes, and other diseases were all higher than predicted this month (by 14%, 7%, 12%, and 9% respectively, or a total of 530); and
- deaths from cancer and dementia were close to expected.
In the full year of 2021, doctor-certified deaths from all causes were around 2,000 (1%) higher than predicted, noting that this is not outside the prediction interval for the year across all causes of death. However, by cause:
- there were 1,217 doctor-certified COVID-19 deaths;
- deaths from respiratory disease were around 2,700 (17%) less than predicted, which is significantly lower than the 2.5th percentile;
- cancer deaths were very close to predicted;
- deaths from dementia were around 490 (3%) less than predicted, which is also lower than the 2.5th percentile;
- there were more deaths than expected from heart disease (up 930 or 7%), cerebrovascular disease (up 420 or 5%), diabetes (up 330 or 7%) and other causes (up 2,500 or 6%), and these deaths were higher than the 97.5th percentile. Higher deaths from these causes exceeded the lower deaths from respiratory disease and dementia.
 Total excess deaths in 2020 and 2021
Total excess deaths in 2020 and 2021
The following table shows our estimate of excess deaths for 2020 and 2021 in respect of ALL deaths assuming that:
- the proportion of doctor-certified deaths from disease (by cause of death) in 2020 and 2021 are the same as for the 2015-19 years, noting that the proportion of doctor-certified diseases has been very stable from year-to-year; and
- predicted deaths from external causes are based on a simple linear projection of the number of such deaths in 2015 to 2019. ‘Actual’ deaths from external causes are estimated from Table 14.1 of the ABS Cause of Death publication, with a similar allowance for late reported deaths from external causes as in previous years (i.e. around a 10% allowance). This results in deaths from external causes being slightly below predicted, which is consistent with preliminary data on the number of deaths from road accidents and suicide.
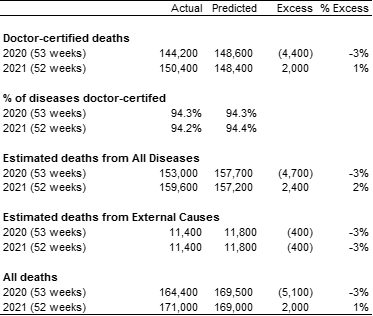
Table 2 – Total excess deaths
|
|
We estimate that total excess deaths for 2020 are around -5,100 (-3%), while for 2021 total excess deaths are estimated to be around +2,000 (+1%).
![]()
COVID-19 related deaths in 2022
While the ABS provisional mortality statistics data is only available until the end of December 2021, the officially recorded COVID-19 deaths are available daily. The following graph shows the number of such deaths in each month of 2020, 2021 and the first three months of 2022.
On 31 March, NSW Health released a report that detailed the outcomes of a reconciliation between their daily death counts and data held by Births, Deaths and Marriages (which is the basis of the ABS data). This reconciliation identified 331 deaths that had not been captured in the daily counts. We have shown these deaths separately.
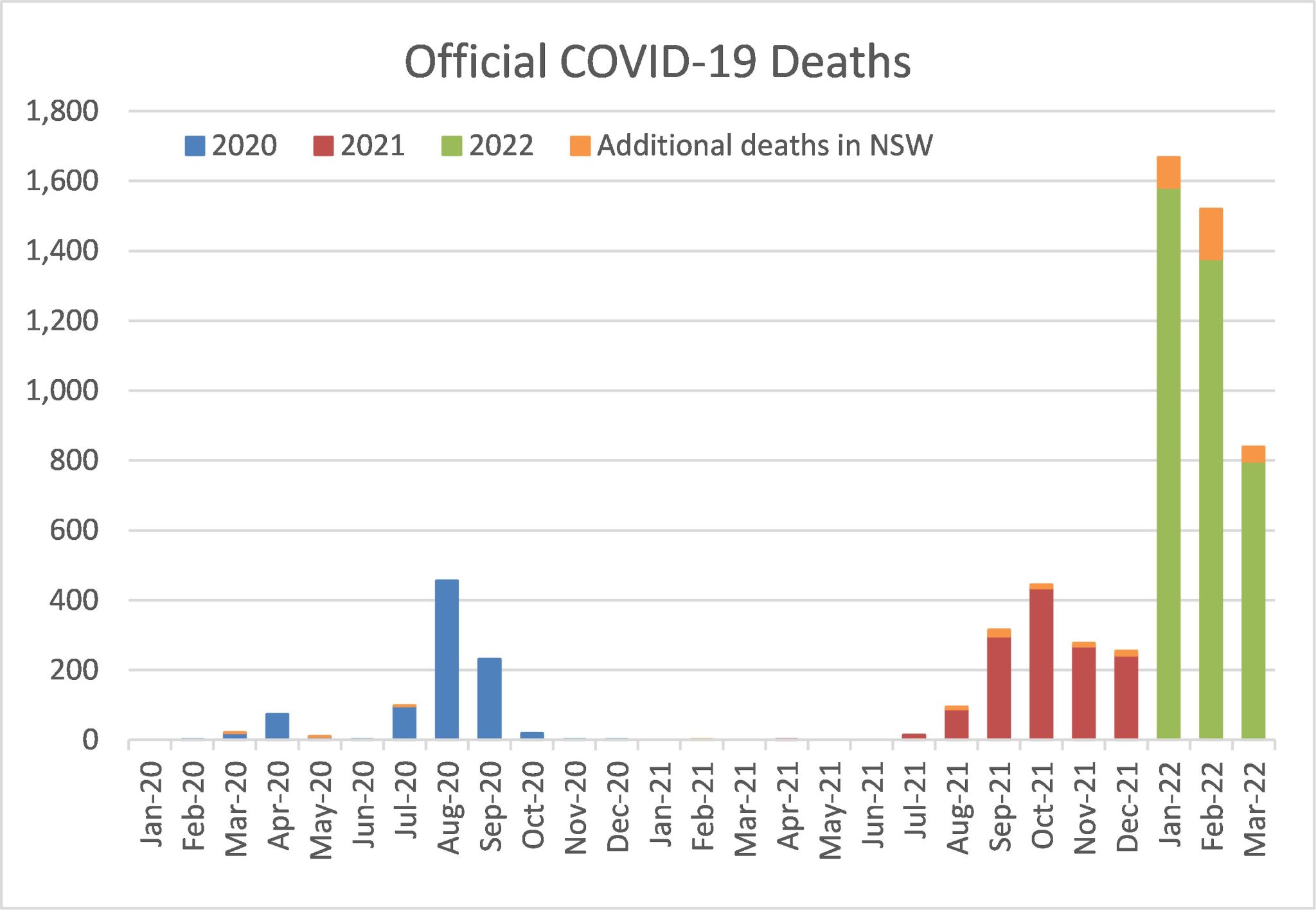
Including the additional NSW deaths, there were 912 official COVID-19 deaths in 2020 (including 854 doctor-certified) and a further 1,402 deaths in 2021 (1,198 doctor-certified). So far in 2022, there have been 4,027 COVID-19 deaths (1,668 in January, 1,520 in February, and 839 in March).
The ABS report Australian COVID-19 Mortality released on 16 March 2021 showed that since the Omicron wave, an increasing proportion of deaths mentioning COVID-19 are in people where COVID-19 is on the death certificate but is not the underlying cause of death. We estimate that during the Omicron wave, 14% of people have died with COVID-19 rather than from COVID-19. Therefore, we estimate that, of the 4,027 deaths reported in 2022, around 3,500 may be due to COVID-19.
Our prediction model suggests that, without a pandemic and including allowance for coroner-referred deaths, there would have been a total of around 40,000 deaths in the first quarter of 2022 (around 13,700 in January 2022, 12,400 deaths in February 2022 and 13,800 in March 2022).
Thus, if mortality from other causes is in line with our pre-pandemic predictions, the COVID-19 deaths will increase excess mortality by around 9% over the quarter (by around 10% in January and February and by about 5% in March).
Combining the excess deaths for 2020 (-5,100) and 2021 (+2,000) with the expected excess mortality in the first quarter of 2022 (+3,500), we can see that deaths from the Delta wave in the latter part of 2021 and the Omicron wave in early 2022 have fully eroded the negative excess deaths experienced earlier in the pandemic.
![]()
Comparison to ABS excess deaths
Table 1 above shows that estimated excess deaths in respect of doctor-certified deaths are:
- -4,400 or -3% for 2020.
- +2,000 or +1% for 2021.
With the release of the full-year data on doctor-certified deaths, the ABS also released an analysis of excess deaths showing -1,734 for 2020 and +5,090 for 2021. It is worth noting a key difference in approach between our estimate of excess deaths and the ABS estimate – we have used data from 2015to 2019 to form and estimate of the expected number of deaths in 2020 and 2021 in the absence of the pandemic. The ABS has used data from 2016 to 2020 to form an estimate of the expected deaths in each year from 2016 to 2021.
- The ABS estimates are not “in the absence of a pandemic”, given that they use the 2020 year in forming their predictions.
- The prediction for 2020 is based on data that includes the 2020 year, so is not formed independently.
- The predictions do not explicitly allow for changes in population size and age distribution, rather implicitly assuming them from prior trends.
A comparison of our estimate and the ABS estimate is shown below.
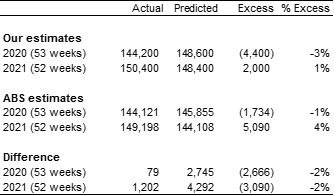
Table 3 – Comparison to ABS (doctor-certified deaths)
|
|
The ABS estimate of excess deaths is around two percentage points higher more than our estimate for both 2020 and 2021:
- Our predicted numbers of deaths are higher than the ABS. This is likely to be largely due to the ABS including the year 2020 (with very few flu deaths) in the predictive model, as well as allowing only implicitly for changes in population size and age distribution.
- Our estimate includes a higher number of ‘actual’ doctor-certified deaths. This is due to our inclusion of an allowance for late-registered deaths.
![]()
Comparison to OWID excess deaths
OWID includes information on all excess deaths in Australia. It draws its analysis from the World Mortality Dataset (WMD) that uses the approach of the June 2021 paper Tracking excess mortality across countries during the COVID-19 pandemic with the World Mortality Dataset by Karlinsky and Kobak. The full database of actual deaths predicted deaths and excess deaths for each country is available on GitHub.
At the time of writing, OWID had not updated its tables and charts to include the month of December 2021, hence we have taken the following figures from the WMD directly.
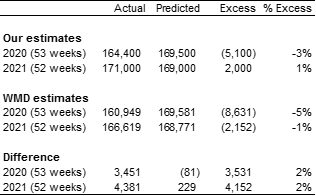
Table 4 – Comparison to WMD (all deaths)
|
|
There is quite a sizeable difference in the excess deaths measured by us and by WMD. The bulk of the difference comes from a difference in the ‘actual’ number of deaths, with our predicted values being quite close.
We have been in discussions with the WMD modellers over the past month or so to try resolve the differences between our estimates. They have made one change that has brought our excess death estimates closer together. The remaining difference stems from the way that WMD modifies the doctor-certified deaths to estimate total deaths, and we believe there is an error in their approach. The ABS have stated that they will be releasing weekly data on all deaths (including coroner-referred) later this month, and the WMD modellers have decided to make no further changes to the Australian estimates until this data is available.
| The remainder of this article shows the actual versus predicted doctor-certified deaths to 31 December 2021 for each cause of death. |
COVID-19 deaths in 2021
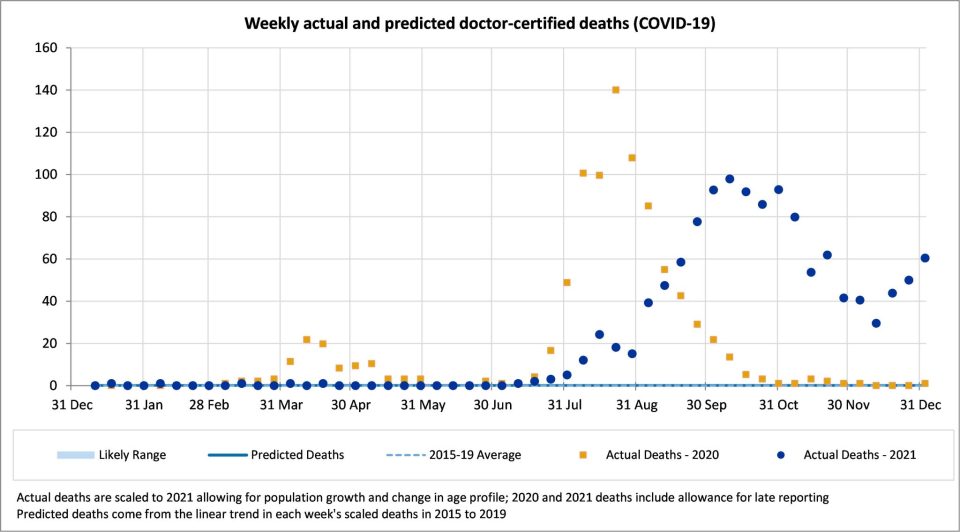
There were 192 doctor-certified deaths in December from COVID-19, compared to the 255 recorded deaths (63 fewer). We would not expect the numbers to be identical, because:
- there are delays between the time of death and lodgement of the doctor’s certificate (noting that we have not made any allowance for late reported COVID-19 deaths);
- the reporting criteria are slightly different; and
- some COVID-19 deaths will be referred to the coroner (e.g. deaths occurring at home).
In the year 2021, there have been 1,217 doctor-certified deaths, compared with 1,402 officially recorded COVID-19 deaths.
![]()
Deaths from respiratory disease
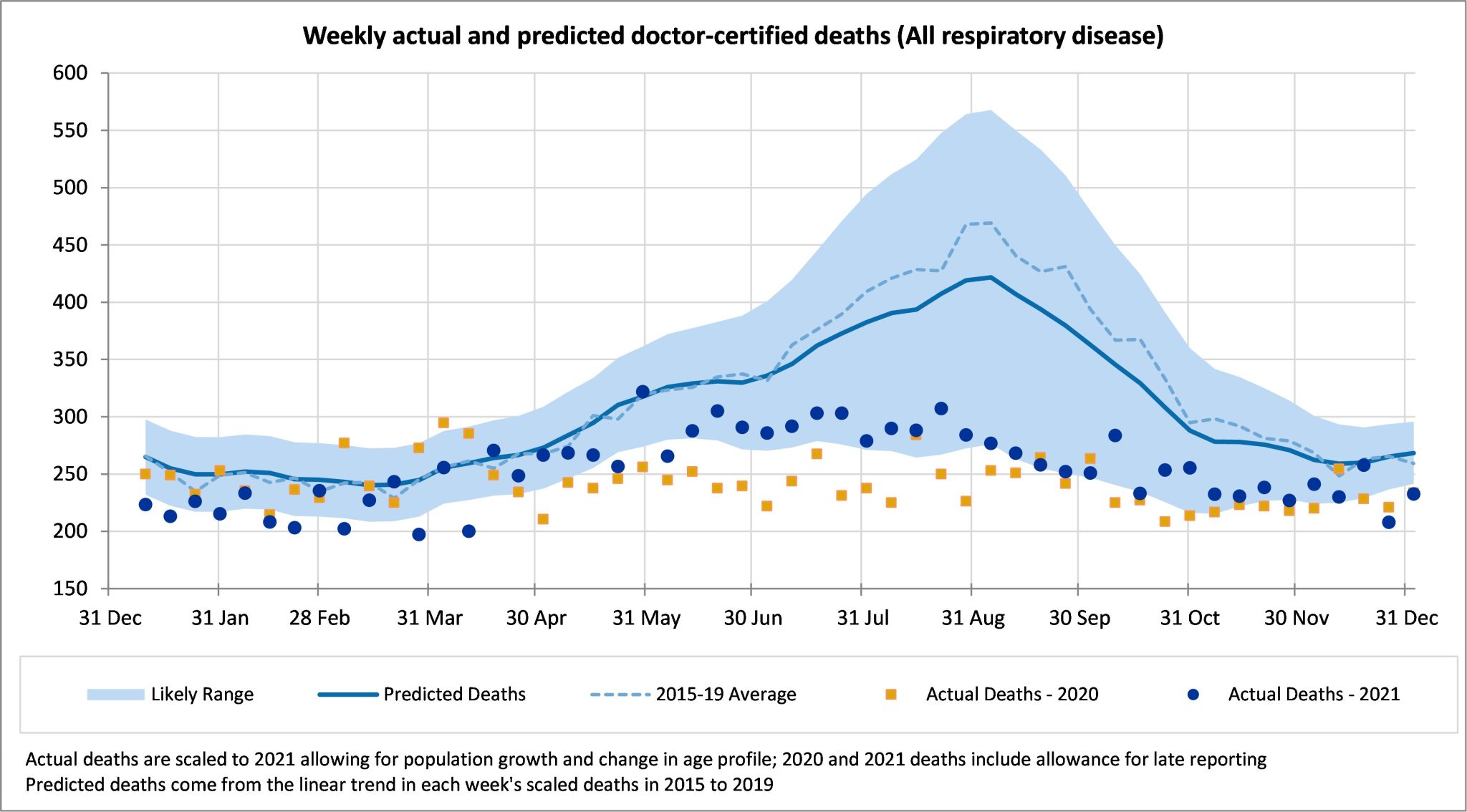
Following the trend observed since the beginning of the COVID-19 pandemic, Australia continued to see lower deaths from all respiratory disease in December 2021. While deaths from respiratory disease continue to be lower than expected, the absolute number of lower-than-expected deaths is fewer than observed during the winter months of July to October.
Deaths from respiratory disease in 2021, while much lower than trend, have been higher than in 2020 for almost all weeks since mid-April.
The following figures present a breakdown of respiratory disease into influenza, pneumonia, lower respiratory disease, and other respiratory disease.
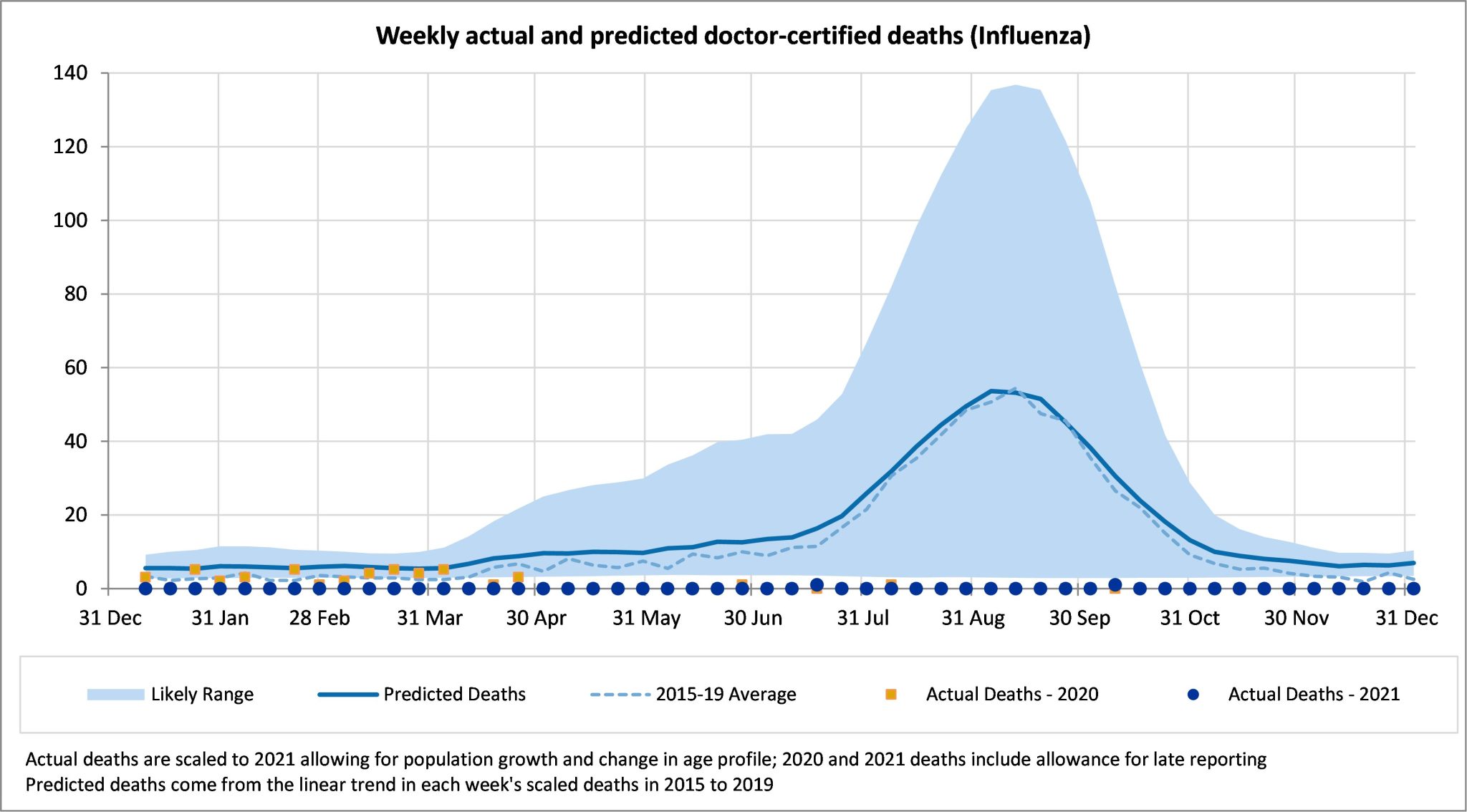
There were no Influenza deaths in December 2021, which means there were only two doctor certified deaths caused by influenza in 2021.
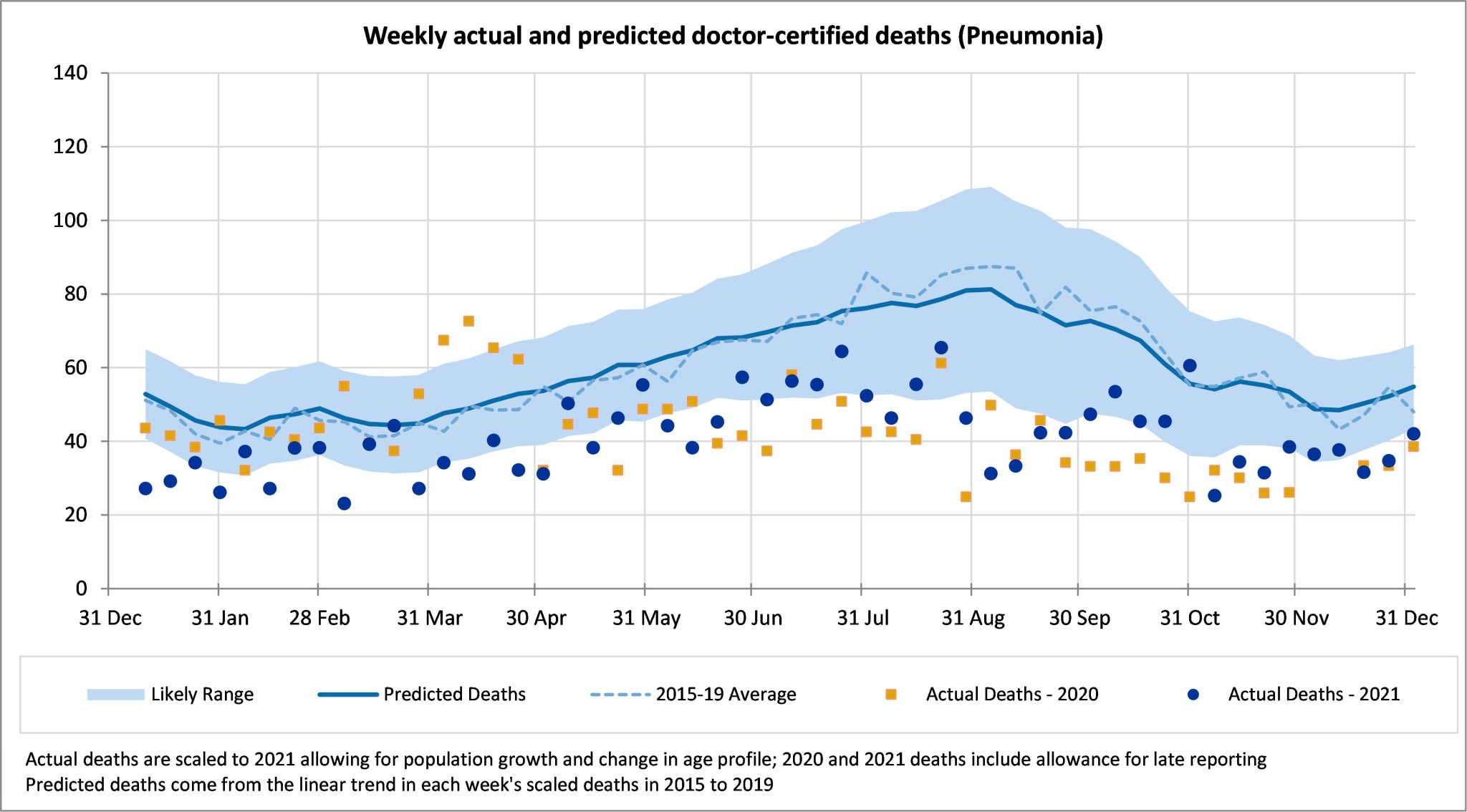
Pneumonia deaths were well below the predicted deaths in December, as they have been throughout the year.
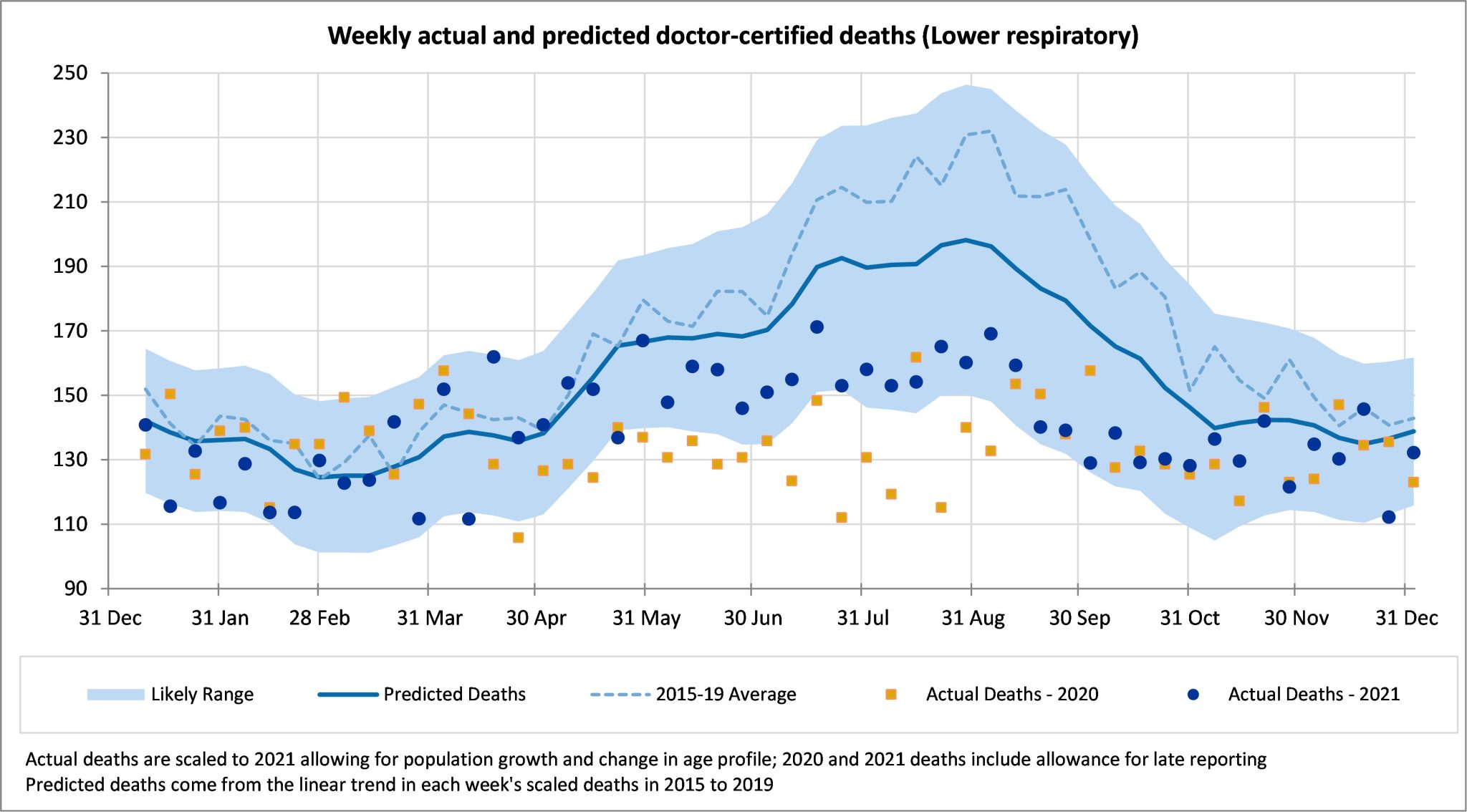
Deaths from lower respiratory disease were lower than predicted in November and December 2021, but not as far below predicted as over the winter months of June to October.
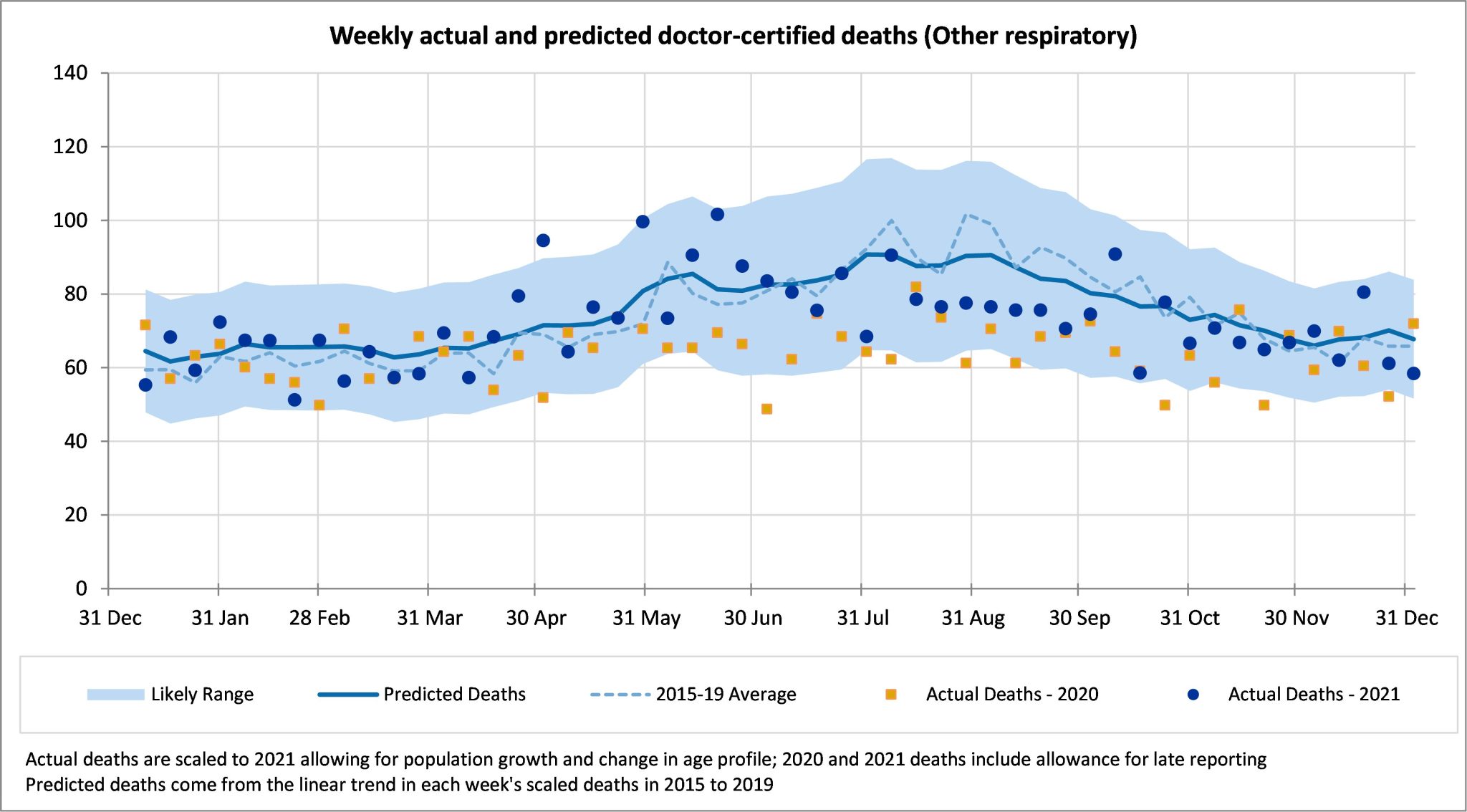
Deaths from other respiratory diseases continue to be close to our predictions with some highs and lows throughout the year.
![]()
Non-COVID-19 and non-respiratory deaths
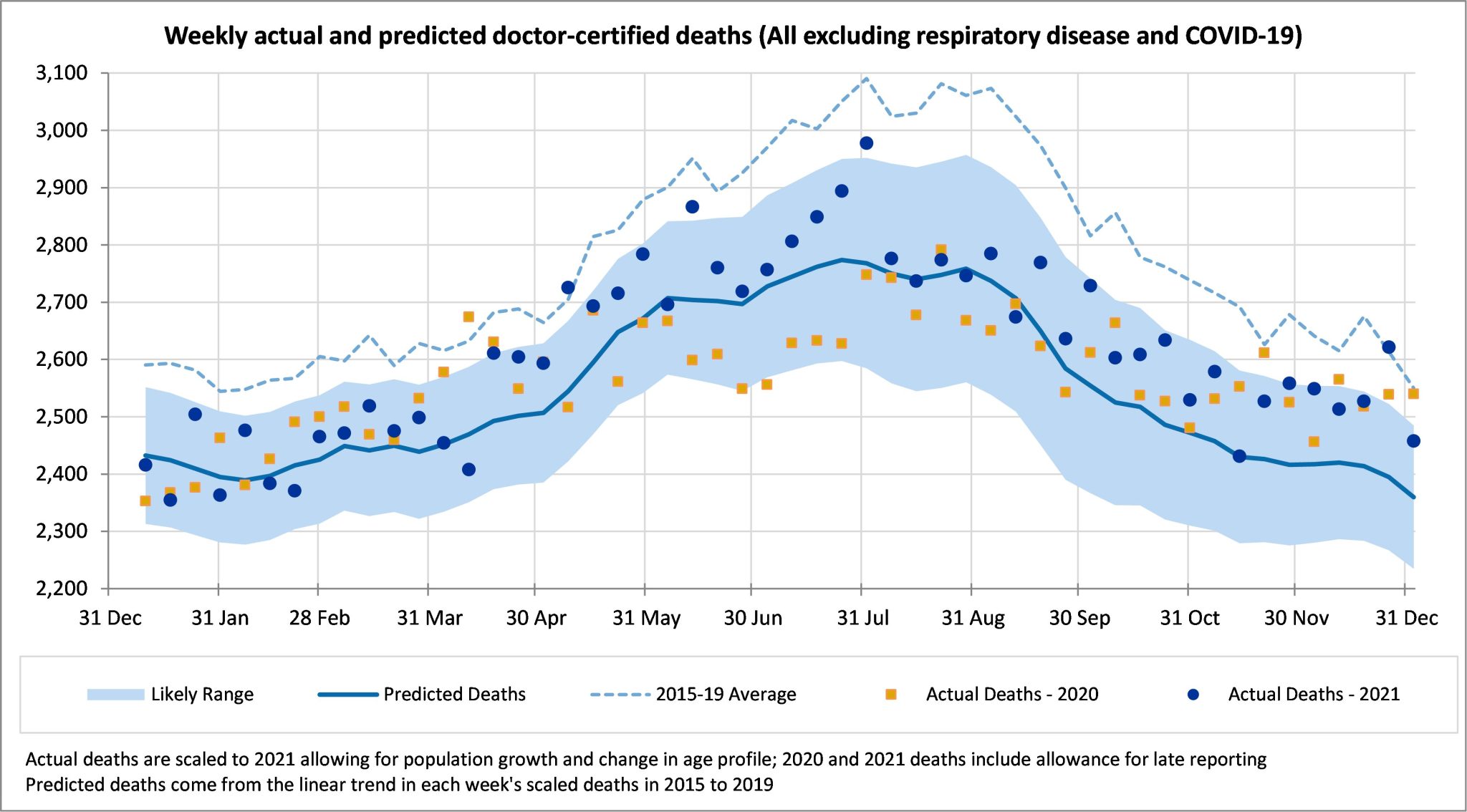
Excluding deaths from COVID-19 and respiratory disease, deaths in December were much higher than expected, and at or above the prediction interval for most weeks. This is mainly driven by much higher-than-expected deaths from heart disease and ‘other’ diseases.
The following figures show a breakdown of non-respiratory/non-COVID-19 deaths into cancer, heart disease, cerebrovascular disease, diabetes, dementia, and all other causes.
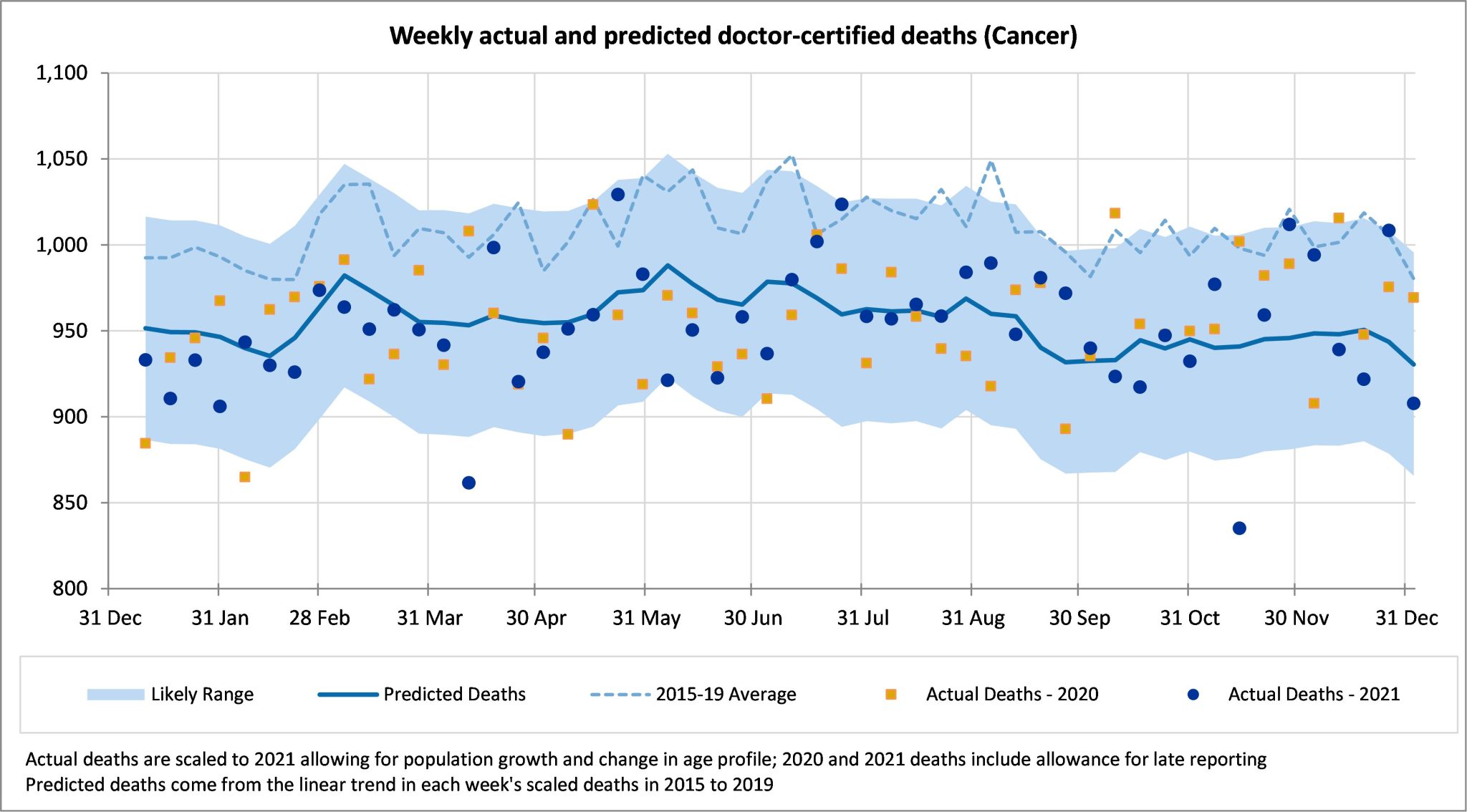
Cancer deaths continue to be close to the predicted values for most weeks. With diagnostic testing down in 2020, there were concerns that there would be a spike in cancer deaths in 2021 and beyond. While it is still early days, we are not yet seeing any evidence of this effect.
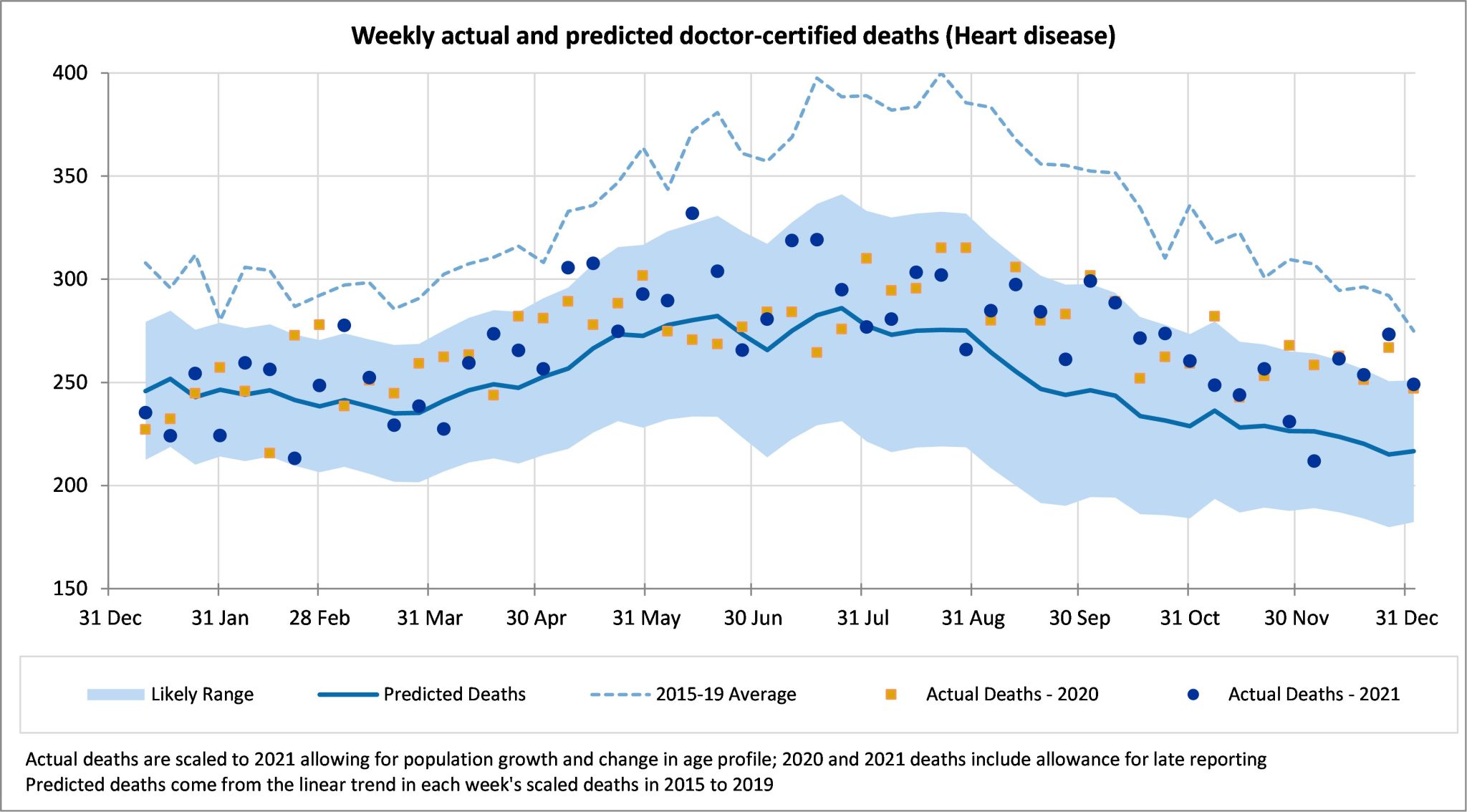
Deaths from heart disease were 14% higher than predicted in December 2021, with four out of five weeks at or above the prediction interval. There are very few weeks in 2021 where deaths from heart disease were lower than predicted, and only three such weeks after mid-April 2021. We note that the predicted values allow for continued strong mortality improvement in 2021 in this cause.
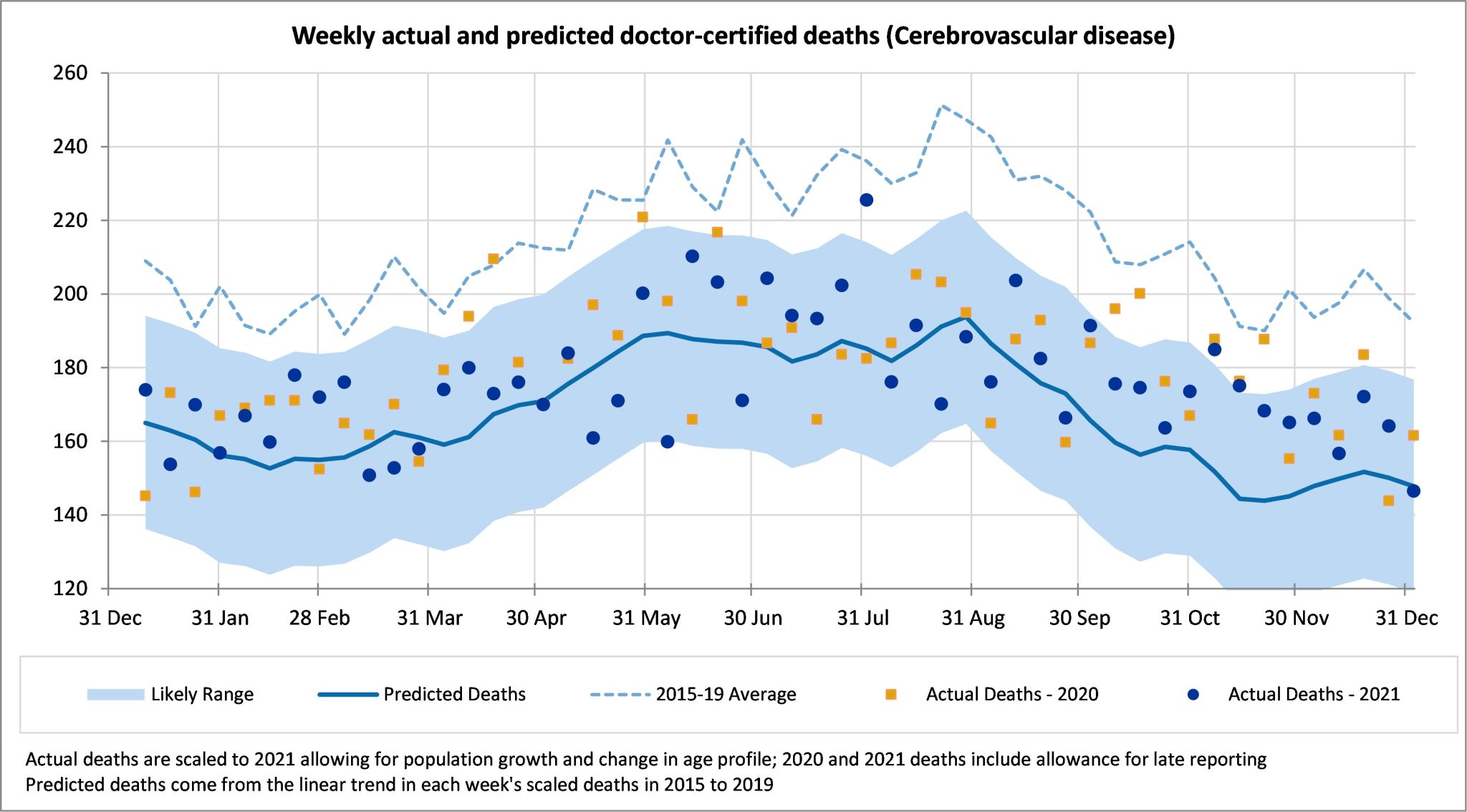
For cerebrovascular disease, actual deaths are 7% higher than predicted across 2021. Most weeks are higher than predicted but are within the 97.5th percentile. Note that predicted values incorporate a continuation of strong mortality improvement.
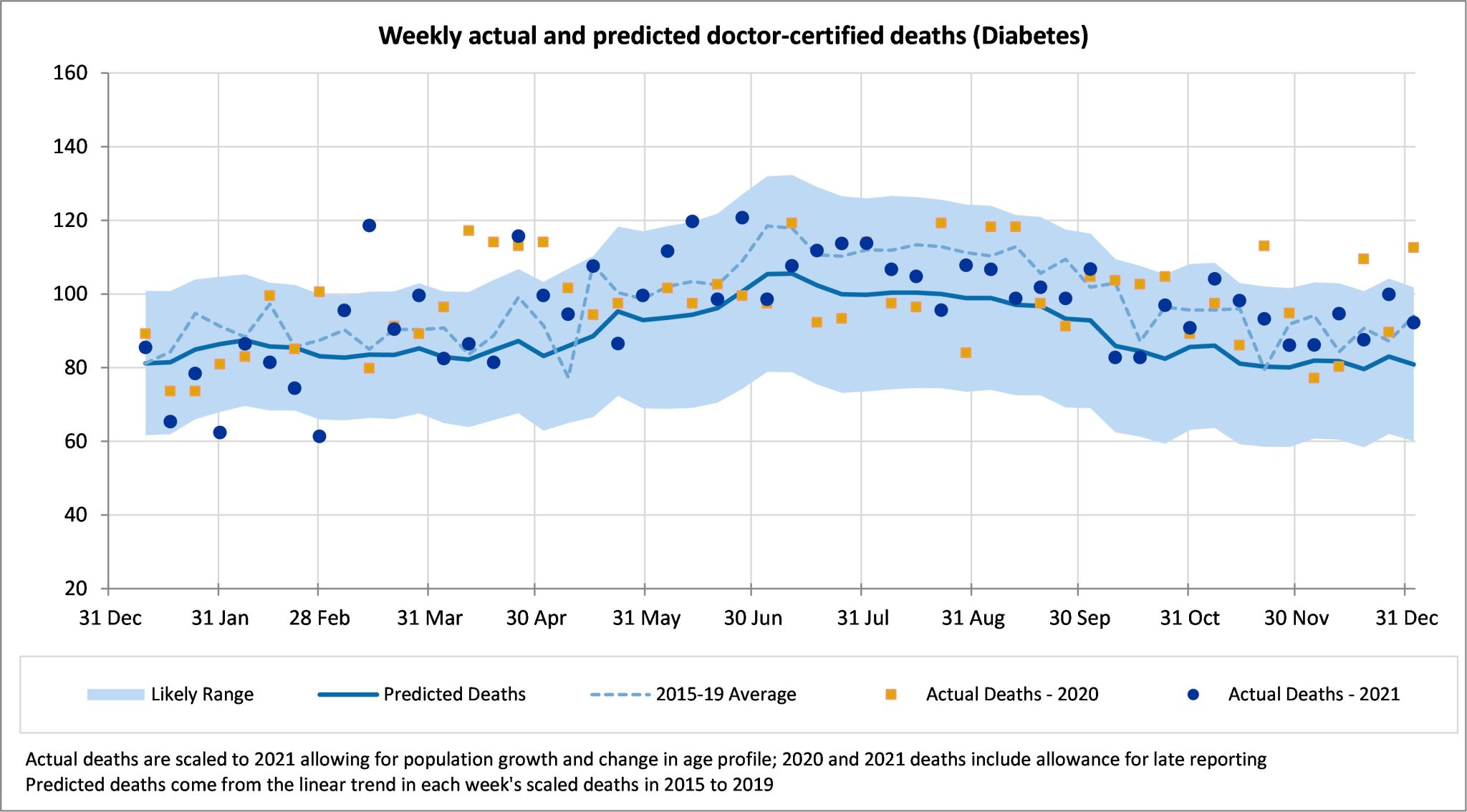
Deaths from diabetes are 12% higher than expected in the last month of the year and 7% higher over the whole of 2021. Deaths from diabetes only make up a small proportion of all deaths, which leads to a somewhat higher volatility, however most weeks are above the mean prediction.
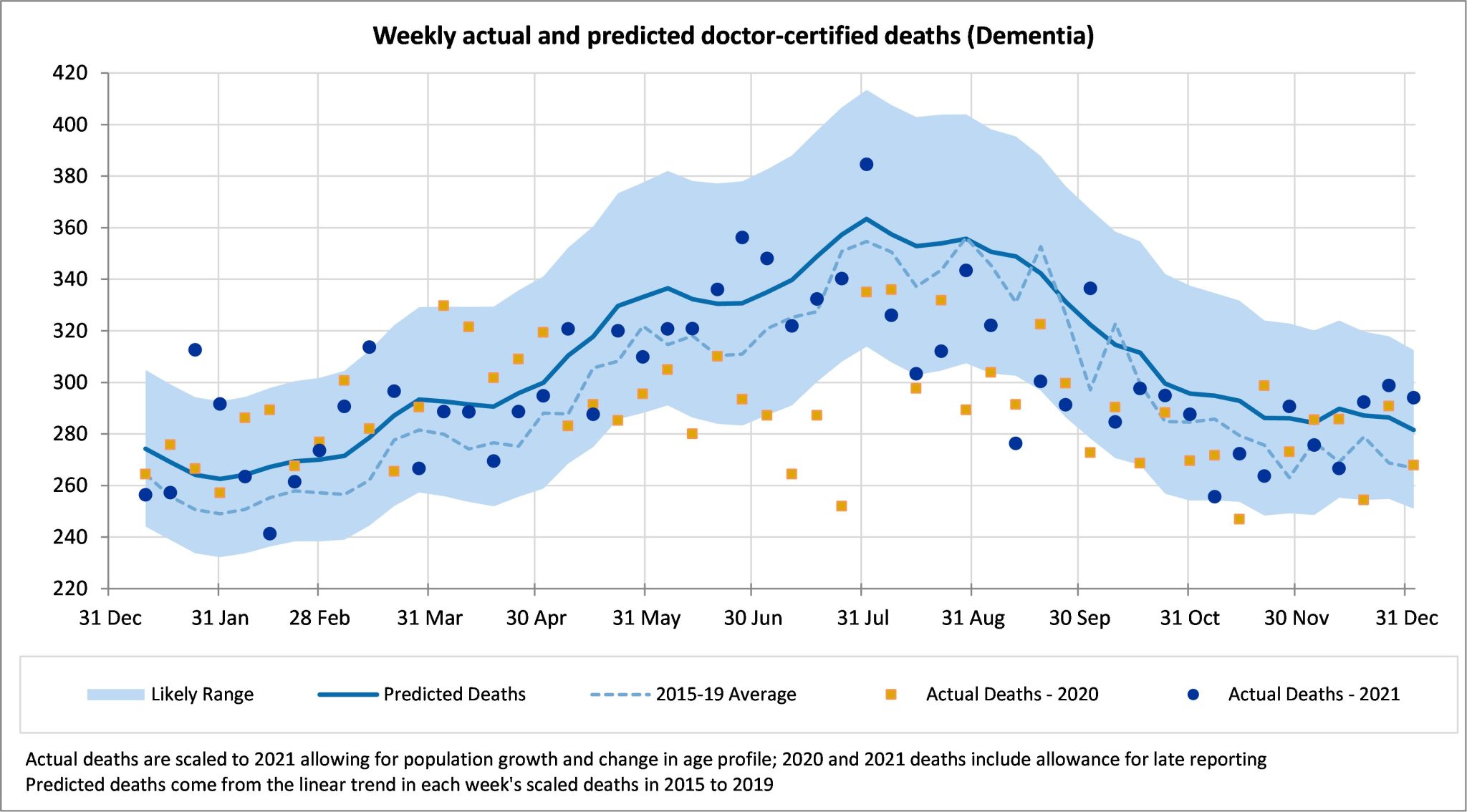
Deaths from dementia were close to expected in the last five weeks of the year. This follows lower than expected experience during July-November and is possibly related to lower than usual levels of respiratory disease in the community.
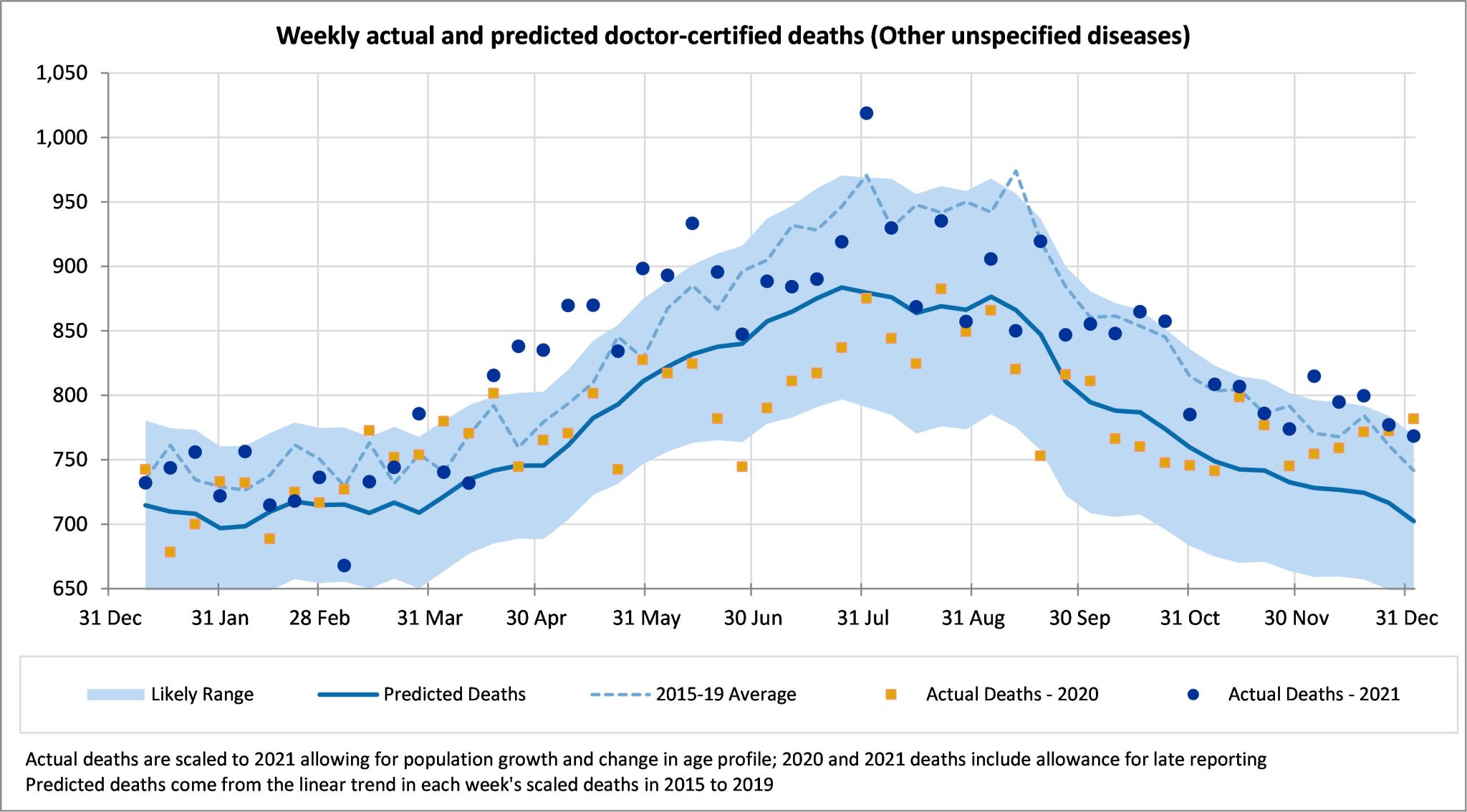
Deaths from other causes, i.e. those not explicitly reported on by the ABS, were again higher than expected in December. In particular, the first three weeks of December were higher than the upper limit of the prediction interval.
|
Members of the COVID-19 Mortality Working Group:
|
CPD: Actuaries Institute Members can claim two CPD points for every hour of reading articles on Actuaries Digital.